Originally published on Smithsonian
The old port town of Bari, on Italy’s Adriatic coast, was bustling. It was December 2, 1943. The British had taken Puglia’s capital in September, and though the front now lay just 150 miles to the north, the medieval city, with its massive cliffs cradling the sea, had escaped the fighting almost unscathed.
Only a few miles outside of town, lines of women and children begged for black-market food, but here shop windows were full of fruit, cakes and bread. Young couples strolled arm in arm. Even ice cream vendors were doing a brisk trade.
Bari was a Mediterranean service hub, supplying the 500,000 Allied troops engaged in driving the Germans out of Italy. Grand waterfront buildings were recently designated the headquarters of the United States Fifteenth Air Force. The liberating Tommies had already chased the Nazis from the skies over Italy, and the British, who controlled the port, were so confident they had won the air war that Air Marshal Sir Arthur Coningham announced that Bari was all but immune from attack. “I would regard it as a personal affront and insult if the Luftwaffe should attempt any significant action in this area,” he said that day at a press conference.
Four days earlier, the American Liberty ship John Harvey had pulled in with a convoy of nine other merchantmen, and some 30 Allied ships were crammed into the harbor, packed against the seawall and along the pier. Their holds were laden with everything from food and medical gear to engines, corrugated steel for landing strips, and 50-gallon drums of aviation fuel. Visible on the upper decks were tanks, armored personnel carriers, jeeps and ambulances. Bright lights winked atop huge cranes that hoisted baled equipment up and out.
At 7:35 p.m.—a blinding flash followed by a terrific bang.
The ancient port’s single antiaircraft battery opened fire. Then came an earsplitting explosion, then another, and another. German Junkers Ju-88s flew in low over the town, dropping bombs short of the harbor. Smoke and flames rose from the city’s winding streets.
As incendiaries rained down on the harbor, turning night into day, gunners aboard the anchored ships scrambled to shoot down the enemy—too late. The attacking German airplanes fled into the night. The raid lasted less than 20 minutes.
Soon a tremendous roar came from the harbor. An exploding ammunition tanker sent a huge rolling mass of flames a thousand feet high. A reporter for Time magazine noted a “fiery panorama.” Eight ships were already “burning fiercely,” he wrote, and the “entire center of the harbor was covered with burning oil.”
A ruptured bulk-fuel pipeline sent thousands of gallons gushing into the harbor, where it ignited into a gigantic sheet of flame, engulfing the entire north side of the port. Flames leapt from ship to ship. Crews worked frantically to free ships before raging fires forced them to jump overboard and swim for it.
The attack on Bari, which the press called “a little Pearl Harbor,” shook the complacency of the Allied forces, who had been convinced of their air superiority in Italy. All told, the Nazis sunk 17 Allied ships and destroyed more than 31,000 tons of valuable cargo. More than 1,000 American and British servicemen were killed, and almost as many wounded, along with hundreds of civilians.
In the crucial days that followed, the task of treating gravely injured sailors would be made even more difficult by wartime secrecy. It would be almost 30 years before the world would learn the truth about what really took place that night, and even today few are aware of the surprising role of the disaster and its impact on the lives of ordinary Americans.
Lt. Col. Stewart Francis Alexander, asleep in his quarters at Allied Force Headquarters in Algiers, was awake at the first harsh jangle of the telephone. There appeared to be a developing medical crisis in Bari. Too many men were dying, too quickly, of unexplained causes. The symptoms were unlike anything military physicians had seen before, and they had begun to suspect that the Germans had used an unknown poison gas. There was an urgent request for assistance. Alexander, a medical officer attached to the staff of Gen. Dwight D. Eisenhower at AFHQ, had received special training in chemical warfare. He was being dispatched immediately to the scene.

Alexander looked young for a combat physician. Five-foot-eight and skinny, he was 29, and only the hair thinning at his temples lent him an air of authority. He was popular with the troops, though some patients kidded that his gentle bedside manner was best suited to a pediatrician. But he had been through the brutal invasion of North Africa under Maj. Gen. George S. Patton, and despite a quiet modesty Alexander had proven himself determined and resourceful.
He could have sat out the war in a stateside hospital or research laboratory, but the desire to serve ran deep. He was descended from self-made immigrants, part of a wave of Eastern European Jews who, fleeing famine and persecution, journeyed to the United States in the 1880s and ’90s and were forever grateful for the opportunity afforded them in their new home. Alexander’s father was an old-fashioned family practitioner in Park Ridge, New Jersey, and Alexander’s one ambition was to follow in his footsteps. After excelling at the Staunton Military Academy, in Virginia, he entered Dartmouth College at age 15. A standout in his science courses, he was allowed to advance directly to medical school in his senior year, graduating at the top of his class in 1935. After completing Dartmouth’s two-year program, he earned his medical degree from Columbia University, and did his residency training in New York. Then Alexander returned home, where he proudly hung his shingle next to his father’s. They enjoyed their shared dream of practicing medicine together for only a few months.
In the spring of 1940, Alexander notified the draft board that he was “available any time.” He was called up in November and spent time with the 16th Infantry Regiment, stationed at Gunpowder Military Reservation, in Maryland, not far from Edgewood Arsenal, home of the Chemical Warfare Service, or CWS. Before long, he contacted CWS with an innovative new design for spectacles that fit within the facepiece of a gas mask. (He was granted a patent on the spectacles, but he turned the rights over to the Army.)

Transferred to Edgewood, Alexander underwent a crash course in poison gases, consulting specialists and experimenting on animals to evaluate toxic agents and forms of treatment; he even investigated agents’ medicinal potential. After Pearl Harbor, he taught Army medical personnel how to treat chemical casualties. He was promoted to director of the Medical Division of CWS’s Research Laboratory at age 27, and when General Patton embarked in October 1942 with 35,000 troops to attack the coast of Morocco, the first time U.S. ground forces would face Axis armies, Alexander accompanied him as the Consultant in Chemical Warfare Medicine to the Western Task Force.
Now, at 5 p.m. on December 7, 1943, five days after the attack on Bari, Alexander’s plane touched down at the city airfield. Waiting for him on the tarmac was the district’s senior British Royal Army Medical Corps officer and a group of hospital directors. “Their agitation was immediately apparent,” Alexander recalled, “and I was taken to the hospital at once.”
The 98th British General Hospital, located in a large complex of brick buildings 15 minutes from the harbor, had been spared. Built on the monumental scale beloved by the Fascists, the Bari Polyclinic housed sizable medical wards, a surgical block and laboratories.
“With every fresh explosion, the building creaked and rattled, rocking like a ship in a storm,” E. M. Somers Cocks, a nurse from New Zealand, recalled of the attack. “Doors were wrenched off hinges, windows were shattered, and the bricked-up windows scattered their bricks like hail.” A concussion blast knocked out the power, plunging the hospital into darkness. They were still sweeping up glass when the wounded began to arrive—hundreds of bloodied sailors suffering from shock, burns and exposure. Almost all of them were covered in thick, black crude oil. The litter-bearers brought up the rear, carrying the grievously injured. These were sailors who had jumped from blazing ships, or swum through pools of flaming oil, and were horribly burned.

With so many patients needing urgent attention, there was no time to get many sailors out of their soiled clothes, so the ward matrons did what they could. The “immersion” cases received a shot of morphine, blankets to keep them warm and strong, hot, sweet tea. Then they were left to rest. A British nurse, Gwladys Rees, remembered trying to fix an intravenous line by the light of a match while the wind blew through shattered windows. “We worked by the dim glow of hurricane lamps, long into the night and early morning,” she recalled. “Intravenous bottles were dripping from every third bed, and the corridors were crammed with patients for whom we could find no accommodation.”
* * *
The first “unusual” indication, the doctors informed Alexander, was that casualties did not present typical symptoms or respond to treatment in the typical manner. Many patients, despite a thready pulse and low blood pressure, did not appear to be in clinical shock. Instead of being restless or anxious, they were apathetic—some even said they felt “rather well”—and their extremities were warm rather than cold.
After dawn, nurses observed that a few of the men complained of being thirsty, even though orderlies had just gone around with the drinks cart. Suddenly there were so many men clamoring for water the whole ward was in an uproar. Patients were yelling about the intense heat, tearing off their clothing, and, in their frenzy, trying to rip off their bandages.
Overnight, the majority of immersion cases had developed red and inflamed skin, with blisters “as big as balloons and heavy with fluid,” Rees recalled. This, together with widespread nausea and vomiting, led doctors to think the cause might be poisonous fumes, possibly from the fuel oil and explosives. “We began to realize that most of our patients had been contaminated by something beyond all imagination,” she said.
Six hours after the attack, patients who had managed to fall asleep awoke complaining of eye pain. They said their eyes felt “gritty, as though sand particles had gotten in,” Alexander wrote in his report. Within 24 hours, the wards were full of men with eyes swollen shut. As the staff’s unease deepened, British naval headquarters sent a notification that there was a “possibility of blister gas exposure” among the casualties. The hundreds of burn patients with unusual symptoms were to be classified “Dermatitis N.Y.D.”—not yet diagnosed—pending further instructions.
Given the crush of casualties that first night, nonurgent cases who had appeared in “good condition” were sent away, sometimes in their wet uniforms. The next morning many returned, clearly needing treatment. Nurses tried to clean them up, scrubbing the black scum from patients’ skin with kerosene, but many took a turn for the worse. “We did everything humanly possible, but it was no good,” Rees said. “It was horrible to see these boys, so young and in so much obvious pain. We couldn’t even give them strong sedatives, since we weren’t quite sure how they would react with whatever had poisoned them.”
The first unexplained death occurred 18 hours after the attack. Within two days, there were 14. Alexander noted the startling downward spiral. “Individuals that appeared in rather good condition in a matter of minutes would become moribund and die,” the doctors told him. The British doctors were mystified. The symptoms did not correspond to case histories of mustard gas poisoning from World War I, or to manuals issued by the Chemical Warfare Service. If the toxic agent was mustard—named for its unpleasant garlicky odor—respiratory complications should have been more prominent.

Several days later, patients with no previous respiratory problems became congested and developed very sore throats, making it hard to swallow. These patients died not as a result of broncho-pneumonia, as might have been expected, but from cardio-circulatory failure.
Alexander walked the crowded wards. He examined patients, gently lifting blankets to study their wounds. With extraordinary delicacy, he probed the strange patches of thickened red skin. He spoke with each patient in turn, asking how he had come by his injuries. Which ship was he on? How did he come to be rescued? Did he receive first aid at the docks? What about at the hospital? One sailor after another told of being caught in the firestorm, of the pandemonium, of somehow making it to the hospital. There they had waited for as long as 12 and even 24 hours before receiving treatment.
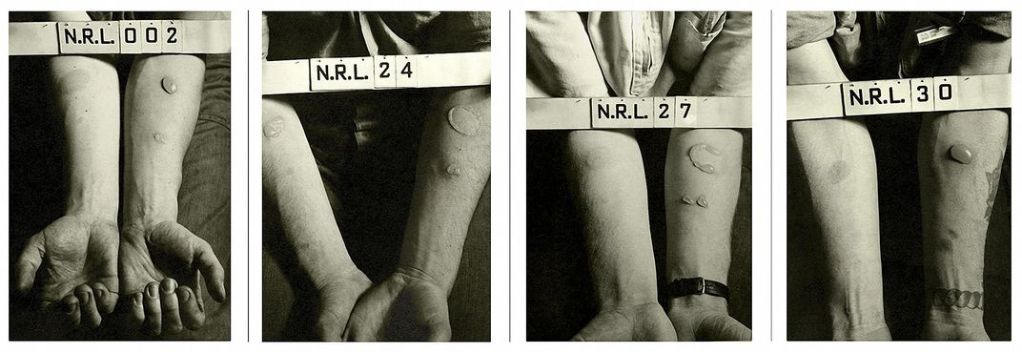
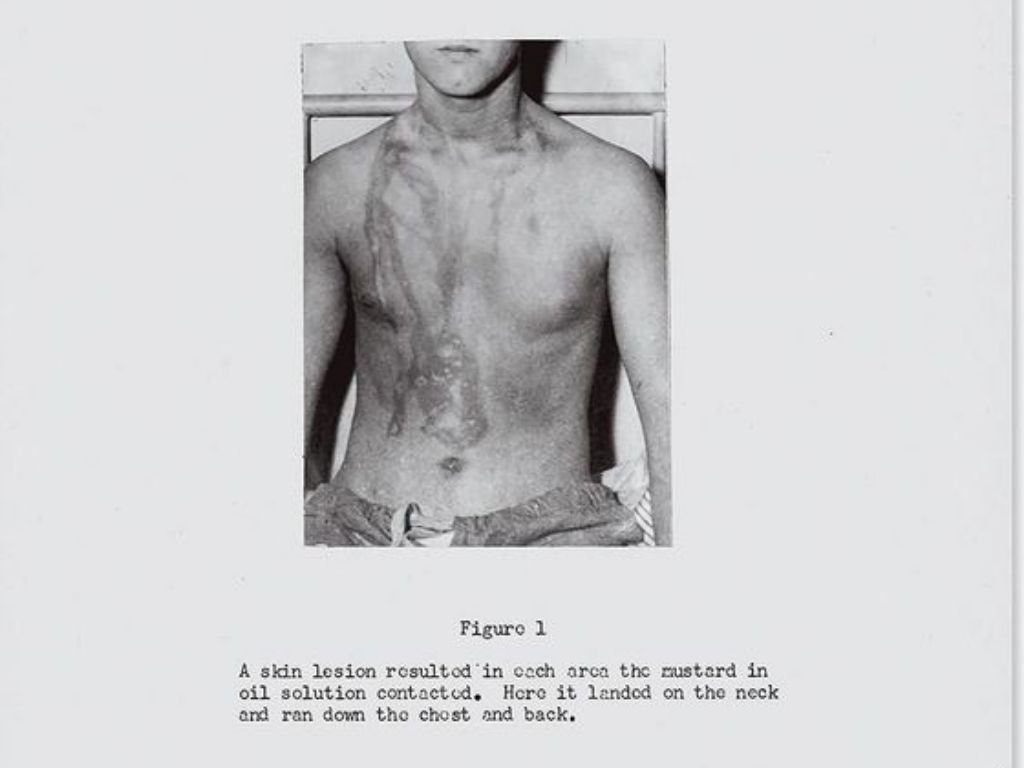
Drawing back the covers from one patient, Alexander studied the burns on an otherwise healthy body. The sailor said he had been aboard a PT boat in the harbor when the German bombers flew over. He heard a loud boom as a nearby ship blew up, and the boat was hightailing it back to shore when he felt a spray of oily liquid land on his neck and run down his chest and back. Alexander observed the outline of raw, raised skin, shiny with ointment, delineating where he had been sprayed, as if the splash had been imprinted on his flesh. The burns Alexander had seen on other patients were varied, but already he could distinguish between chemical burns and those caused by fire and heat: “Certain patterns were present depending on how the individual had been exposed.”
It appeared to Alexander that sailors who had been thrown overboard and completely immersed in the harbor were burned extensively, while those in boats had comparatively superficial burns wherever the toxic soup had hit them. Several men who had sat in the solution, possibly in lifeboats, had only local burns of the buttocks and groin. A few lucky souls who took it upon themselves to wipe off the oily mixture that first night sustained only minor injuries.
As he made his rounds, it was increasingly clear to Alexander that most of these patients had been exposed to a chemical agent. His sense of smell supported his hypothesis. Entering the hospital, he had noticed something different from the usual cloying mix of sweat, urine and disinfectant. “Traces of an odor implanted in my mind said mustard gas,” he later recalled.
He knew that the three most common blister agents were sulfur mustard, lewisite and nitrogen mustard. Although generally referred to as “gas,” all three agents were liquids at room temperature. And all three produced skin injuries resembling burns and serious eye injuries. Particularly worrying was the new, pure-grade nitrogen mustard developed by the Germans, which Alexander had studied the previous year, at Edgewood, after two classified samples were smuggled out of Germany. Its effects were reportedly more rapid than sulfur mustard, and it could penetrate intact skin and cause systemic poisoning. Practically colorless and odorless, apart from a faint fishy smell, it was not easily detected in the field. The Germans were also known to use mixtures of blister agents, so any combination was a real possibility.
It had been five days since the initial exposure, and if there was any chance of saving the hundreds of Allied sailors lying in hospitals all over Bari, plus countless Italian civilians, he would need to act swiftly.
He decided to put the question directly to the commanding officer of the 98th General Hospital, Col. Wellington J. Laird. “I feel these men may have been exposed to mustard in some manner, Colonel,” Alexander said tentatively. “Do you have any idea how this might have happened?”
“None,” came Laird’s reply.
As the chemical warfare consultant to, Alexander was cleared to the “highest degree.” He knew the Allies had begun secretly stockpiling poison gas in the Mediterranean, in case Germany, with its back against the wall, resorted to all-out chemical warfare. But he was skeptical that the Allies would have shipped mustard shells into a busy port like Bari and allowed the toxic cargo to sit there as a prime target for an enemy strike. Still Alexander couldn’t rule it out. Tactfully, he tried again. “Have you checked with the port authorities?” he asked Laird. “Could the ships in the harbor have been carrying mustard?”
Laird replied, “I have, and they tell me they have no such information available.”
The burden of proof rested on him. He ordered a series of tests for the patients who were still alive, and insisted on “careful and complete autopsies” on patients who had died under mysterious circumstances. He ordered samples of the harbor waters collected and analyzed. He borrowed personnel from displaced hospital units and put them to work gathering data, performing lab tests on tissue samples and compiling pathology reports.
Suspecting that Laird had dodged his question, Alexander visited Navy House, the British admiralty’s local headquarters. Weary after the long day, he was blunt: Was there mustard gas in Bari Harbor? This was again “absolutely denied.”
Alexander left unconvinced. What he needed was proof. But this was not the familiar menace he had studied at Edgewood. This was a new horror, “mustard gas poisoning though in a different guise than that recognized from WWI,” he wrote later.
At first light, Stewart Alexander headed for the harbor. He picked his way through mounds of rubble and surveyed the twisted skeletal remains of the Allied convoys. Out on the mole, men were working like ants, removing jagged chunks of concrete and scrap metal. The port, which had been closed for five days and swept for mines, had partially reopened that morning. A number of burned-out vessels had already been towed out to sea and sunk or blown apart. A coal barge still smoldered on a quay close by, and the fly ash stung his nostrils.
The dark oil-slimed water in the harbor basin looked sinister. One sailor had recalled that the floating oil had been a foot thick on the surface of the water after the raid. It was a mixture of high-octane gasoline and fuel from two dozen Allied ships and, Alexander suspected, mustard gas or a derivative, possibly dropped by the Germans among the incendiary bombs. Alexander wondered what other agents might have been thrown into the mix. The Germans possessed phosphorus and magnesium bombs, both of which would have caused deep chemical burns and eye injuries. Another possibility was that an Allied cargo ship had been carrying white phosphorus shells and smoke pots—designed to mask approaches and unnerve the enemy—which were released when the vessel was hit.
If it was an aerial gas attack, determining which ships were hit and in what order would help him understand which crews suffered the most direct exposure. Even men not on the water would have inhaled significant doses of the noxious vapor as it spread across the harbor—some of it sinking, some burning, some mixing with the tons of oil floating on the surface, and some evaporating and mingling with the clouds of smoke and flame. German planes could have dropped time-fused mustard bombs that would burst open approximately 200 feet above the water or, in a low-altitude “spray attack,” could have released liquid mustard from tanks that would then have been transformed by the slipstream into tiny droplets resembling a vapor. Alexander reasoned that in either case the attack would have contaminated all the ships in the inner harbor, including the crippled vessels that remained afloat, and drenched all the men on the docks below.
Yet Alexander had found no evidence of mustard contamination in his survey of the dock area. And the Royal Navy personnel he interviewed appeared shocked at the suggestion that poison gas might have been released in the air raid. “Mustard?” one British officer repeated in surprise, shaking his head. “That’s impossible. There’s no mustard here.”
When he spoke with British port authorities, they continued to “state categorically that there was no mustard in the area.” Undeterred, Alexander described in detail the ghastly burns he had seen at the hospital, and he insisted there was no way those injuries could have been sustained by anything except chemical exposure. Of the 534 men admitted to the Allied hospitals following the attack, 281 were suffering from symptoms consistent with mustard poisoning. That day, 45 had died. These were just the documented cases. Many more fatalities could be expected if they did not receive proper treatment urgently. The vast majority of the victims were British—their own countrymen.
The authorities began to waver. They allowed that if mustard gas was present in the harbor, “it could only have come from the German planes.” Alexander considered the ramifications of the charge that Hitler, in a desperate gamble, had risked a gas offensive. But coming as it did after a string of firm denials of so much as a whiff of mustard in Bari, it seemed to Alexander too neat an explanation.
For days he pored over the clinical records. “Reading the reports,” he wrote, “is to take a journey into the nightmare of the effects of chemical contamination.”
From his training, Alexander knew that agents such as mustard are toxic in vapor or liquid form when they reach the eyes, nose, lungs or gastrointestinal tract. But the chemicals can also be absorbed by the skin. And any toxic agent in contact primarily with the epidermis would, therefore, result in delayed clinical signs—as was the case with the baffling Bari victims.
These were the symptoms he bore in mind as he studied the case of Seaman Philip Henry Stone, a patient who had abruptly died after asking for a drink. The doctors had pointed to him as an example of one of the inexplicable “early deaths.” The pathologist noted “a generalized dusky erythema,” or reddened skin, on the chest, abdomen and thighs, and many blisters on the face, ears, arms, back and external genitalia. “The lips were dull black in color,” he wrote.
During the autopsy, the pathologist also found that the esophagus displayed a “curious black longitudinal streaking,” probably due to dead cells and tissue. The lungs, a mottled blackish-red color, were congested, the bronchi were filled with pus, and the trachea engorged with fluid. The stomach showed the same black areas, and there were necrotic areas near the opening, most likely caused by swallowing a diluted solution of mustard mixed with oil.
After studying the reports, Alexander concluded that many sailors who sustained blast injuries would not have succumbed to the hemorrhages were it not for other complications: “The serious consequences of imposing the mustard vapor injury upon a lung partially damaged or bruised by blast is at once apparent.”
Alexander was still trying to decide how best to proceed, given the official resistance to his diagnosis, when he received stunning news. A diver he had ordered to search the harbor floor had found fractured gas shells. Tests performed on-site revealed traces of mustard. Ordnance officers from the U.S. Air Force identified the casings as belonging to a 100-pound M47A2 mustard gas bomb. German mustard gas bombs were always marked with the distinctive Gelb Kreuz, or yellow cross. This bomb was definitely American.
Alexander’s instincts were right—an Allied ship, later identified as the John Harvey, had been carrying a cargo of mustard gas. The secret shipment had most likely been destined for a chemical stockpile at Foggia, 75 miles away, in order to improve the U.S. capability to retaliate against a German chemical attack.
As Alexander knew from his training, the M47 bomb was made of simple sheet metal, designed to hold white phosphorus or liquid sulfur mustard. Although the M47A2 model was coated inside with an oil to protect it from corrosion caused by the agent, the bombs were still fragile. They would have been blown to pieces in the German bombardment, releasing lethal mustard into the atmosphere and the oily harbor water.
Alexander found it hard to believe that this was the first time British officials were learning of the chemical weapons. The circumstances of the accident would need further investigating, as would the extent to which the military authorities had covered up the escaped gas. By failing to alert hospital staff to the risk of contamination, they had greatly added to the number of fatalities. At that moment, however, Alexander’s patients took precedence. Now that his suspicions were confirmed, he could advise the staff at Allied hospitals on proper treatment for mustard exposure and try to reduce the number of deaths.
Instead of bringing matters to a close, however, Alexander’s discovery that mustard gas had come from the Allies’ own supply had made a difficult job that much more complicated. The British port officials’ attempts to obfuscate rankled, but that paled in comparison to their effort to shift responsibility to the Luftwaffe. It was not a harmless fabrication. Alexander shuddered to think about the “grave political implications.” He later recalled thinking, “If they were going to accuse the Germans of dropping mustard when the Germans had not….”
Earlier that year, President Roosevelt had issued a stern warning that any Axis use of chemical weapons would be followed by the “fullest possible retaliation.” The significance of “any error in interpreting the factor of and source of mustard gas in Bari,” Alexander recalled, “was horrendous.” If the Allied leaders drew the faulty conclusion that the enemy had deployed chemical weapons, it could trigger widespread chemical warfare.
Adding to his anxiety, the daily death toll from mustard contamination, which had started to decline, suddenly spiked, demonstrating the secondary effects of pneumonia on patients already weakened by chemical exposure. There seemed no way to predict how many more men would die.
Nine days after the bombing, Alexander gave his initial findings to AFHQ in Algiers. “The burns in the hospitals in this area labeled ‘dermatitis N.Y.D.’ are due to mustard gas,” he asserted. “They are unusual types and varieties because most of them are due to mustard which has been mixed into the surface oil in the harbour.”
Alexander felt growing urgency that his diagnosis be recognized at the highest levels. Some British medical personnel appeared to be waiting for an official stamp of approval before implementing his treatment strategies. More important, there could be no misunderstanding the source of the mustard. He sent high-priority cables to both the American president and the British prime minister, informing them of the nature of the casualties at Bari and the almost certain origin of the gas on an American Liberty ship. Roosevelt appeared to accept his findings, and responded: “Please keep me fully informed.”
Churchill, however, sent a terse reply: He did not believe there was mustard gas in Bari.
Alexander was speechless. He admired Churchill, and he speculated that the British leader’s overriding concern was that the Allies “not acknowledge we had poison gas in that theater of operation because if the Germans retaliated they would be dropping poison gas on England.” There was no questioning the wisdom of this command decision, but Churchill’s opposition undermined Alexander’s credibility and ability to do his job.
Alexander sent a second telegram. He cited his findings at much greater length, stating “beyond any doubt” that these casualties were due to mustard exposure. He was informed that Churchill maintained that “the symptoms do not sound like mustard gas,” which Churchill had witnessed firsthand during World War I. His instructions were the same: “The doctor should reexamine his patients.”
Flummoxed, and unsure how a “lowly, lonely American medical officer” was supposed to respond, Alexander appealed to the liaison officer for advice. The man advised him: One did not argue with the prime minister.
* * *
After a sleepless night, Alexander returned early to the hospital determined to prove there had been no mistake about his diagnosis. Churchill was a brilliant man, with an uncanny instinct for the salient fact, and he had put his finger on the most important question about the Bari victims: Why were the toxic effects so much more serious than any other recorded in military history? Far more patients were dying of mustard symptoms at Bari than on the battlefields of WWI, when the fatality rate had been around 2 percent. The death rate in Bari was more than six times higher—and climbing.
The difference, he believed, was the amount of mustard absorbed through the skin from the unprecedented, intimate and lengthy contact as a result of being immersed in the oily harbor water, and then left to sit in soaked uniforms. “In this group of cases,” Alexander postulated, “the individuals, to all intents and purposes, were dipped into a solution of mustard-in-oil, and then wrapped in blankets, given warm tea, and allowed a prolonged period for absorption.”
Alexander’s medical inquiry into mustard’s effects on the victims was just beginning. As he sat reviewing the case sheets and pathology reports, one recurring observation leapt out at him: the devastating effects on the patients’ white blood cells. He flipped through a stack of records. There it was again and again—the white blood cell counts fell off sharply. In patients who recovered, white blood cell concentrations corrected by the second or third day; but in some cases, the white blood cell count dropped precipitously beginning on the third or fourth day. He noted that lymphocytes, the white blood cells found in the lymph organs and of importance to the immune system, “were the first to disappear.” What he was looking at made the hair on the back of his neck stand on end. Alexander had seen these exact results before, but never in human beings.
In March 1942, the authorities at Edgewood, having received the nitrogen mustard compounds smuggled out of Germany, turned the samples over to Alexander to investigate their impacts on the body. Alexander and his colleagues immediately began detailed experimental protocols on animals. The first studies, which recorded the effects of exposure on the skin, eyes and respiratory tracts of rabbits, showed results that were completely in line with exposure to sulfur mustard in the past and with what was expected from a highly toxic agent of this kind.
Next, they set up an experiment to determine the effects on the blood and blood-forming organs. Twenty healthy rabbits were exposed to lethal doses of the agent. To the research team’s astonishment, the white blood cell count of the rabbits dropped to zero or points very close to zero. No one at the lab had ever seen such rapid destruction of white blood cells and the accompanying deterioration of lymph nodes and bone marrow. The researchers consulted the literature and found no reports of the same kind of reduction of white cells in the blood, known as leucopenia, or anything that had the same effect. Alexander’s first thought was that they must have a “bad batch of rabbits.” But when they repeated the experiment with a new group, the results were the same.
Alexander ordered the tests repeated with other lab animals to rule out the possibility of poor stock or species sensitivity. They tried guinea pigs, rats, mice and goats. Each time, they achieved the same dramatic effects: sudden, severe leucopenia, severe lymphopenia, lymph node depletion and marrow depression. After exposure, the white blood cell counts rapidly disappeared, and the lymph nodes were almost completely dissolved, left as “shrunken little shells” of what they had been.
While still at Edgewood, Alexander was fascinated by the idea that mustard interfered with the body’s mechanism for producing blood cells, especially white blood cells. Because of the dramatic and reproducible effects, he could not help but wonder about the possibility of using the compounds directly, or in modified forms, on human beings with diseases of the blood. If nitrogen mustard attacked white blood cells, perhaps it could be used to control leukemia, the most common type of cancer in children, with its unrestrained white blood cell growth, by using different dosages to destroy some but not all excess cells without annihilating patients. But when Alexander proposed an ambitious set of experiments into mustard’s medicinal properties, he was told first by his chief, and then, on appeal, by the National Research Council, that this was not the remit of the Edgewood laboratory. There was not enough time or money to pursue collateral lines of investigation that did not facilitate the national defense. He was ordered to put the project aside and return to his work on mustard casualty management, treatment and decontamination. Chasing miracle cures would have to wait until after the war.
Now, sitting in an Allied military hospital 6,000 miles away, not even two years later, Alexander held in his hands incontrovertible evidence: “mustard gas did, in truth, selectively destroy blood cells and blood-forming organs,” he wrote. Doctors and medical researchers had never before encountered such an extraordinary level of sulfur mustard toxicity, which, when it mixed with the oil dumped into Bari Harbor, approximated the damage done by the experimental nitrogen mustard compounds—and allowed its systemic effects to be seen clearly for the first time. It had taken a freak accident, and the massive exposures of wartime, to verify in people the phenomenon demonstrated in laboratory rabbits. “It all added up to the same conditions I had seen in my prewar animal work,” Alexander later recalled. “Blood cells disappeared, and lymph nodes just melted away.” He remembered thinking, “If nitrogen mustard could do this, what could it do for a person with leukemia or lymphosarcoma?”
Alexander could not save the worst of the Bari mustard gas casualties, he knew, but perhaps he could make their deaths count for something. A one-in-a-million chance had landed him, one of the few doctors in the world who had studied mustard’s curative potential, in the middle of a disaster with a morgue full of case studies. It was an unthinkably rare chance to perform a pioneering investigation into the toxin’s biological effects on the human body—the kind that would be impossible with living volunteers.
He ran down the hall, yelling for more blood tests. He made sure special care was taken in preparing specimen samples to send to Edgewood for microscopic examination, and improvised a fixative solution, hoping the tissue specimens would withstand the long journey. The hematological analysis would not be as complete as he would like. The heavy burden carried by Allied combat hospitals, and the limited facilities, would prevent them from conducting important tests, including studies of bone marrow and blood chemistry. Alexander would need to be scrupulous in gathering as much data as possible, and in badgering lab technicians to do what he felt was necessary. This time, he wanted to make absolutely sure that his insight into the systemic effects of mustard was entered into the medical record, with an eye toward seeing whether the substance could be used not to destroy, but to heal.
* * *
On December 27, 1943, Lt. Col. Stewart Alexander submitted his preliminary report on his ten-day investigation of the Bari Harbor catastrophe. It was immediately classified. Eisenhower and Churchill acted in concert to keep the findings secret so there was no chance Hitler could use the incident as an excuse to launch a gas offensive. Any mention of mustard gas was stricken from the official record, and the medical staff of the British hospitals in Bari were instructed to alter the patients’ charts. Alexander’s diagnosis of toxic exposure was deleted and replaced with the generic terminology for combat casualties—burns, lung complications, all other injuries and deaths “due to enemy action.”
The feared German chemical attack never came. The Wehr-macht was deterred by logistical constraints, combined with Allied air superiority and the threat of massive retaliatory strikes. Ironically, the Germans had known all along about the source of the poison gas in the harbor. Nazi spies in the port had suspected that the Allies might be concealing mustard bombs among the munitions they were stockpiling in Italy. After the air strike, they sent down their own diver, an Italian frogman loyal to the Fascists, who recovered a fragment of an M47 bomb casing, which confirmed the chemical weapons were American.
British officials never acknowledged Alexander’s Bari report, but it garnered high praise from Eisenhower’s senior medical advisers. They lauded the exceptional job Alexander had done under challenging conditions, but told him that a commendation was withheld for fear of “offending the Prime Minister.” Nevertheless, Col. Cornelius P. “Dusty” Rhoads, chief of the Medical Division of the Chemical Warfare Service, hailed Alexander’s meticulous investigation as so complete, and of such immense value to medicine, that it represented almost “a landmark in the history of mustard poisoning.”
Rhoads was eager to explore the toxic agent’s therapeutic potential. Like Alexander, he believed the Bari data pointed the way toward a promising new chemical targeting white blood cells that could be used as a weapon in the fight against cancer. Rhoads, who in civilian life was head of New York’s Memorial Hospital for the Treatment of Cancer and Allied Diseases, seized on the wealth of new information provided by the Bari victims as a breakthrough. His ambitious plans for Memorial Hospital now converged with Alexander’s report and crystallized into a single mission—to exploit military research into poison gas to find a chemical that could selectively kill cancer cells.

Armed with the Bari report, and the results of a top-secret Yale University trial that demonstrated for the first time that a regimen of intravenous nitrogen mustard—in tiny, carefully calibrated doses—could result in human tumor regression, Rhoads went in search of funding to develop this experimental treatment, known today as chemotherapy. He persuaded Alfred P. Sloan Jr., the chairman of General Motors, along with the company’s wizard engineer, Charles F. Kettering, to endow a new institute that would bring together leading scientists and physicians to make a concentrated attack on cancer. On Tuesday, August 7, 1945, the day the world learned that an atom bomb had been dropped on Japan, they announced their plans for the Sloan Kettering Institute for Cancer Research. World War II was over, but the war on cancer had just been launched.
The official secrecy surrounding the Bari disaster continued for decades. The military refused to acknowledge the chronic effects of mustard exposure on hundreds of surviving sailors, naval personnel and civilians, resulting in years of suffering, controversy and lawsuits for medical compensation in both the United States and Britain. In 1961, Alexander volunteered to help the National Academy of Sciences conduct a study of the American survivors, but the project stalled when identifying victims of contamination proved too difficult. “All the records said ‘burns due to enemy action,’” recalled Alexander.
Alexander was discharged from the Chemical Warfare Service in June 1945, and returned home with a chest full of medals and battle ribbons, as well as a new bride, Lt. Col. Bernice “Bunny” Wilbur, the highest-ranking Army nurse in the Mediterranean Theater. He turned down Rhoads’ offer to work at the fledgling Sloan Kettering Institute. Instead, he kept his promise to his father to continue their family practice in Park Ridge, New Jersey, where he became a much beloved physician and cardiologist, and where he raised two daughters with Bunny. He served for 18 years as director of the Bergen Pines County Hospital, and taught at the medical schools of Columbia and New York University. He never boasted of his wartime exploits, but he always took quiet pride in his unique contribution to medicine, and did not mind that while many textbooks eventually traced the modern age of chemotherapy to the Bari disaster, the details of his investigation remained enshrouded in secrecy. He died on December 6, 1991, of a malignant melanoma—skin cancer—but not before the U.S. Army belatedly commended him, three years earlier, for his actions during the Bari episode. “Without his early diagnosis and rapid initiation of appropriate and aggressive treatment, many more lives would have been lost and the severity of injuries would have been much greater,” the commendation read. “His service to the military and civilians injured during this catastrophe reflects the finest measure of a soldier and physician.”


